Perioperative Care Instruction Guide
Perioperative Care Instruction Guide
*This is just a guide and should clarify or supplement our preoperative discussion about what to expect and do. It should not replace any specific instructions we covered together as they pertain to your specific medical condition(s) and needs. Do not hesitate to call the office anytime.
First of all, thank you for trusting me in your care! I hope you have a smooth and fast recovery!
Below are the typical instructions I give to my patients as well as answers to some common questions that I receive from patients after surgery. I hope this will guide you through your recovery period.
At any point in your recovery if you have an emergency call 911. If you have questions or concerns that are NOT emergent, please contact our office at (470) 419-4380. If you call during normal business hours a member of our team will likely be able to address your concerns directly. If they can not, they will relay the message to me, or one of my highly trained experienced partners, to call you back. Please be patient with us in returning your call.
I like to break down post-operative recovery instructions into categories as follows: Post op medications, diet, activity, wound care and follow-up plans.
Medications:
*Note that NOT every single medication is covered in this section. Some common examples are provided. We should have covered the medications before surgery and if we have not, please contact me.
Most likely it is safe and expected that you take your usual home medications leading up to the day of and after surgery. Most routine surgeries do not require a major change in medications but we do know that some medications, especially after a major surgery or a long surgery, can affect your recovery and potentially cause complications. There are some categories of medications that need special attention.
The major categories of medications to consider around surgery are anticoagulants (blood-thinners), antiplatelets, antihypertensives (blood pressure meds), and diabetic medications.
Anticoagulants/antiplatelets:
If you are taking any medication in the “anti-platelet” or “anti-coagulation” category PLEASE MAKE SURE THAT WE HAVE DISCUSSED THE PLAN FOR THIS MEDICATION BEFORE CONTINUING. Common medications in this category include Aspirin, Clopidogrel (Plavix), Ticagrelor (Brilinta) Warfarin or Coumadin, Lovenox, Eliquis, Xarelto or others. You could have a serious bleeding complication if you take these medications the day before surgery or restart these medications too soon after surgery. We should discuss preoperatively when to stop and or what alternative medication to take leading up to surgery. I will fill out paperwork on your discharge instructions from the hospital after surgery, indicating if and when to restart the medications.
Antihypertensives:
Although they do a good job controlling high blood pressure normally, occasionally during or after surgery they can cause problems. This is because during and after surgery you could have significant “fluid shifts.” In response to the surgery, fluids in our body tend to “shift” from the blood vessels out into other organs and tissues. You will almost assuredly get IV fluids the day of surgery as well. Furthermore powerful general anesthesia medications will be on board and sometimes it is hard to predict your body’s response to and the time needed to clear these anesthesia drugs. So post operatively these antihypertensive medications you commonly take could cause unintentional but dangerous decreases in blood pressure and these changes can come as a sudden change to the heart and even the kidneys too.
The major classes of antihypertensive medications are diuretics, ACE inhibitors and Angiotensin Receptor Blockers (ARBs).
Common diuretics include Hydrochlorothiazide (HCTZ), Chlorthalidone, Furosemide (Lasix), Bumetanide, Amiloride, Spironolactone (Aldactone). Common ACE Inhibitors are Lisinopril (Prinivil, Zestril), Captopril, Enalapril (Vasotec), Benazepril (Lotensin). Common ARB’s are Valsartan, Losartan, Irbesartan, Olmesartan.
As before unless otherwise discussed, generally it is recommended that these classes of medications can be taken (as the last dose) the MORNING PRIOR to the day of surgery. Do not take the medication the morning of surgery. I will fill out paperwork on your discharge instructions from the hospital after surgery, indicating if and when to restart the medications.
Diabetic medications
There are many types of oral and injectable diabetic medications. How to tailor insulin doses will come primarily from your prescribing, or primary care, doctor’s recommendations. When fasting for surgery your blood glucose levels can fluctuate and or drop suddenly especially if you take certain diabetic medications while fasting. Beyond the possible hypoglycemia, or low glucose, from taking a diabetic medication during fasting there are other potential complications to your body during recovery. Particularly medications in the Sulfonylurea class, such as Tolbutamide or Gliclazide, should be held on the day of surgery. Megletide class drugs, like Repaglinide, and SGLT-2 Inhibitors like Dapagliflozine should be held the day of surgery as well. Thiazolidinediones like Pioglitazone should be stopped for at least one day before the day of surgery. Metformin is a common medication that should also be stopped for one day prior to surgery. I will fill out paperwork on your discharge instructions from the hospital after surgery, indicating if and when to restart the medications.
*As a special note, if you are having weight loss surgery it is very likely that we stop all antihypertensives and diabetic medications after surgery however if we have not discussed your medication plan already, do not use this guide exclusively, and please contact the office.
Diet:
*Note, if you are a weight loss surgery patient, you need to refer to the extensive review materials provided by our team of dieticians and plan to follow the pre and post operative diet guidelines within.
*Note, if you had an antireflux surgery or surgery specifically on your stomach or intestine then you likely will have more specific diet instructions. If you are finding this hand out and we have not discussed a diet plan, then plan to stay on clear liquids (which is always a safe first option after surgery) and call the office.
If you are like many patients, you have not experienced true hunger in a long time. So fasting is a major source of duress for most patients and believe me I do not take pleasure in keeping patients without food or drink. However, fasting before surgery is a safety related recommendation driven by the anesthesiology team and it is mandatory to follow their guidelines. Following the rules preoperatively and following the recommendations below for after surgery will maximize the chances of having a safe, smooth surgery and recovery experience.
Generally speaking, after most of the surgeries I perform it will not be harmful to resume your usual diet. Your post op diet instructions will likely say “regular diet.” However, I tell my patients to go slow and listen to your body. After all you just had a big surgery. I tell my patients to treat themselves like mom would have treated them if they were sick with the flu.
You should wait until you have had a couple of hours of rest at home without nausea or gas pain before advancing the diet, even if you passed the diet test at the hospital. You may have had medications on board for nausea at the hospital and things may have changed. Focus on non-carbonated oral hydration first when you get home and then try something like a light soup with toast or Jello with crackers for that first meal. Walk some if you can and wait for true hunger pains. While it is hard to predict each person’s response to surgery, there is no doubt in my mind that if you go slow and eat a light first meal without trouble, then you are more likely succeed in advancing that diet to normal. If you are passing flatus after surgery then that is an even better sign that you will not have a problem going forward.
The reason I recommend moving cautiously is that I have had patients call with nausea and vomiting after trying to eat a regular meal as soon as arriving home. If you rush to eat you could have retching which will cause new or worse incisional pain. This cycle can quickly become a set back. Finally please note that if you are having terrible nausea and or vomiting despite taking it slow, then it could be a side effect of one of your mediations (very common with narcotics especially) or something else. Please call the office to discuss your symptoms with us if you are not able to keep liquids down.
Activity
Your discharge instructions will likely say: “Activity as tolerated, but no lifting >20lb or straining until your follow up appointment. Try not to strain even on the toilet. Use stool softeners as needed if getting constipated.”
Activity after surgery is one of the best things you can do to get back to normal quickly. Return to normal activity is optimized by minimally invasive surgery techniques which is why I love doing what I do.
Walking helps keep the lungs open and clears fluid build-up. It also helps the stomach and intestines return to normal function faster. It can help reduce the risk of blood clot formation in your leg veins. However activity can be over done too. I have had patients after weight loss surgery whom were too eager to begin exercise and have had significant complications. Below I will give some recommendations for acceptable activity levels. First however let me review the likely limiting factor in your activity, which will be pain.
The first place you will feel pain after surgery is not your abdomen that much actually. There is different type of pain unique to minimally invasive surgery that we call referred pain. This pain originates in the abdomen but is “referred” to the shoulders instead. This pain is from the carbon dioxide gas we use to inflate the abdominal cavity. That pain is felt at one or both of your shoulders. Most patients will remember this pain more than any other pain in the recovery room and for up to 12 hours or so after surgery. The carbon dioxide gas irritates the diaphragm muscles. The nerves that control our diaphragm muscle, because of the way our nerves develop, share some connections with the sensory nerves near our shoulders. So that irritating gas in the abdomen is felt near our shoulders. The best way to clear that gas is actually to be active and walk after surgery.
The second place you will have pain is of course the abdomen itself and at the incisions. One reason that you will not feel this as much right after surgery is that we always finish surgery by injecting the incision sites with a local anesthetic, or a numbing medication. When available we use a long-acting anesthetic medication called Exparel. This medicine has properties that allow it to stay in the tissue near the incision for up to two or three days! Ideally the numbing medicine lasts long enough that you have made it through the most inflammatory part of healing, which is about two or three days after surgery. Pain can feel worse 2-3 days after surgery but rapidly and steadily improves after that point.
While the incisions may be small on the outside, the incisions may be larger on the inside and may even have a deep stitch in place at the level of the muscles. Also note that the inner part of the incision may not be directly under the outside visible incision. Although the incisions are on the skin, the instruments we use go through all the layers, including the muscle layer, of your abdomen. The abdominal muscles are very special. They are not just a six-pack for show. These muscles which were violated by surgery comprise your core and are used to do literally every activity of daily human life. So of course you will be sore when you use those muscles to sit, stand, walk, turn or even take deep breaths or cough, for example. Pain after minimally invasive surgery is most commonly described as “very sore” like “I’ve done a 1000 sit-ups.” There is occasional “sharp” pain, especially when you do something somewhat suddenly. The sharp pain is likely to be at the incision with a deeper muscular stitch. While we want to keep pain controlled please know that to a certain degree of pain is normal and should not deter you from trying to be active.
As with the diet I generally recommend that whatever you do, that you do it slow and listen to your body. After surgery I strongly encourage that you do not go home and stay in bed. Spend a few hours the day of surgery at least sitting up in a chair. Ideally you should be trying to walk around your home at least one to three times (not including necessary bathroom trips) that first day back. For the first 1-3 days after surgery this is what I would expect everyone to do, but each day you should be able to walk a little further and more frequently within the home. You can climb stairs after surgery if you were doing so normally before surgery. Just go slow and take a break every couple of steps and consider having a friend or family around, especially the first day after surgery. By day 4 or 5 most people say they are “turning a corner.” You should try to walk outside to the mailbox and back at this point. By one week post operatively most people say they are “starting to return to usual activity.” Usual home activity means waking up, getting dressed, preparing breakfast, walking around the house freely and cleaning counters without feeling prohibited.
Work and exercise activity
If you have a desk job or can work from home you can probably resume work. Of course if usual activity for you means lifting weights, running long distances, or you have a labor intensive job like construction, you will not be back to usual activity. Most patients by their 2 week follow up tell me this: “I had a pretty normal week so far until I decided to pick up a bag of soil in the garden (or something like this).” This is because by two weeks most people mentally are back to normal but, your body may still lag. Some new level of strain, even if it’s normal strain, can set off inflammation and pain at the incisions.
By two weeks post operatively I usually will tell my patients to advance your activity methodically as you try to resume normal activities. However any activity that causes sharp pain at one or more of your incisions should be avoided for another week before you try again. The painful incision is your activity guide so to speak.
What you definitely should not do is dedicated core exercise (sit ups, for example) for at least another 3-4 weeks. It is possible to apply enough force to tear that deep stitch which of course will be painful. It is rarely an emergent problem but you could also be at risk for an incisional hernia developing if the incisions are not allowed to heal completely. Therefore, if you are an exercise enthusiast I usually recommend supplementing aerobic exercise (jogging for example) to keep burning fat until that 4 week mark. If you must lift weights, I will recommend trying modified workouts to protect the core from sudden violent strain. We can review acceptable workouts at the follow up appointment.
Lastly if you did not get an abdominal binder post operatively then I do recommend you obtain one, especially if you feel incisional pain with activity. Remember your incisions on the outside and the inside are not aligned. So when you engage those core muscles the other layers of the abdominal wall shift around and this can cause inflammation to flare up and could even cause muscle spasm. The binder with mild to moderate tension will support the skin and soft tissue layers against the core and prevent some of this shifting. The binder is not mandatory and can be off or loose when sitting or sleeping.
Wound Care
*If you had open surgery or surgery for an infection you will have very specific wound care instructions.
If you had an outpatient minimally invasive surgery my typical post operative orders usually say, “Okay to shower in 24 hours after surgery, just no soaking or bathing the incisions until the follow up appointment and incision check.”
Note that all the incisions have stitches under the skin that dissolve. The outer most layer of our skin can heal remarkably fast. Usually on average about 24 hours after surgery, the body will put a water tight layer of new skin cells over the incision, but not everybody heals the same. That’s why we reinforce the skin and protect it with different types of dressings. The top most layer of the incision closure will either be an advanced topical skin adhesive (AKA “skin glue”) or small thin adhesives called steri strips. If you have skin glue then there will not be any extra dressing or bandage placed over the incision. If you have steri strips however, there will be one more layer of dressing/or bandage on top of this. It is normal for some fluid and or blood to leak from the incisions post operatively. The dressings are there to collect this initial leakage.
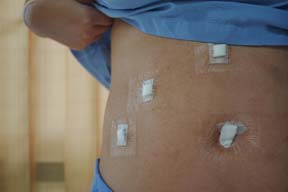
Above is an image of incisions covered with steri strips and simple tegaderm dressing on top of that.
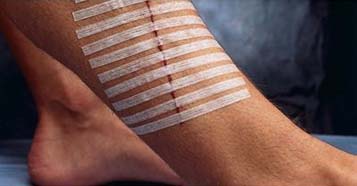
Here is a picture of steri strips on an incision. These are the little strips you want to pat dry over and try to maintain until follow up. (Picture from: https://justhomemedical.com/products/3m-steri-strip%E2%84%A2-adhesive-skin-closure-strips-reinforced-sterile)
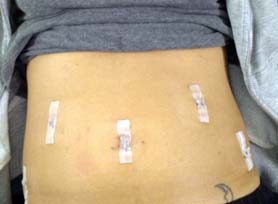
Here is another picture of steri strips on an abdominal incision. These are the little strips you want to pat dry over and try to maintain until follow up. (Picture from: http://postfibroidsurgery.blogspot.com/2012/11/week-6day-37-sunday.html).
Regardless of whether or not you have skin glue or steri strips, you can shower a full 24 hours after surgery. If you have a dressing on you can take that off first, but try to leave the steri strips on. When showering, plan to mostly let soapy water run over the incisions the first couple of showers. Then it is okay to scrub very gently around the incisions but still do not scrub vigorously directly on the incisions at any point. Plan to pat dry over the incisions and again, do not rub vigorously on the incisions with a towel either. I tell my patients to let the skin glue fade by itself and if you have steri strips try to protect them and let them fall off by themselves. If the glue has faded or those steri strips have fallen off before the follow up, it is almost never a big deal. Below we will discuss incision changes that should prompt a call to our office.
Usually at the two week follow up after I check the incisions I will tell you to peel off the skin glue in your next warm shower, or if you still have steri strips I will take these off at the appointment myself.
Probably the most common reason that patients call the office is because the incisions are concerning in some way. Incisions can evolve differently for different patients as they heal. Certain changes can be alarming but rarely are a true emergency requiring a visit to the ER. You can always call the office to discuss incisional changes and can even email us images to make decisions securely and conveniently. My work email address is vishdanthuluri@capitalsurgeons.com, but make sure you call before you email to make sure I am available to review and reply.
The following guide is to help alleviate some stress and to act as a starting point in taking care of yourself until you can discuss with someone in the office. The bottom line is that you should always call first and let us know about the changes.
Bleeding
If your incision is bleeding do not panic. Most of the time it is a skin edge bleeding and due to some activity or shifting around, a previous clot which had formed has been disrupted. There are no named vessels at the level of the skin incision that can cause you to bleed to death unexpectedly. So do not panic! Call and let us know as soon as you can, but plan to first apply some pressure to keep things from getting worse. Most likely after we discuss I will ask you to plan to remove the wet dressing and apply a new dressing or folded paper towel to the area and press firmly for about 15 minutes. If you are able to and can pinch your incision from above and below gently, that may be better. Don’t push or pinch so hard that you are in significant pain. You usually do not need heavy pressure. If it has stopped bleeding after this, plan to reapply a dressing or bandage and take it easy for the rest of the day. If the bleeding is still going on but slower, that means the pressure is working but you need more time. Plan to place another folded gauze or paper towel over the area and hold direct pressure or pinch again for 30 minutes this time. Then, If not already using your abdominal binder you can apply this over the folded gauze to continue to keep light pressure there the rest of the day or night. If your incision is on the arm or elsewhere, an Ace bandage wrap can also hold and maintain the pressure for longer periods. Depending on the results we can decide what to do next. After two attempts to stop bleeding if it has not stopped I will either have you report to our office if able to, or to an ER if it is after hours.
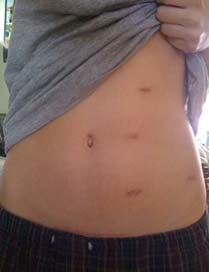
Common incisional changes:
- Note the little bit of pink/red skin changes right near the incision edges. Mild redness the first 1-3 days after surgery is likely normal. This is a very normal looking incision. (Image taken from: https://images.app.goo.gl/XWxWmsvBMNuXBMAVA)
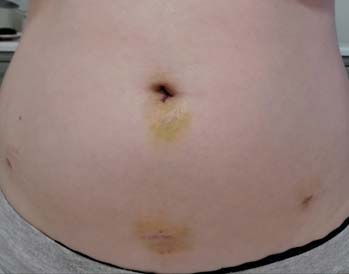
2. Note the yellowing. This is evolution of a small bruise associated with the incisions. The colors can be dark purple or maroon too. Also very normal and not alarming without other symptoms. (Image taken from: https://images.app.goo.gl/io6ufjVAzyZKYStA9 )
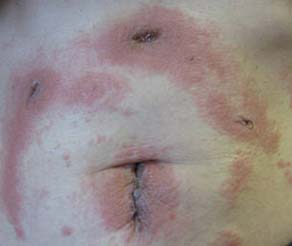
3. Note the redness that is right around all the incisions and spreading between the incisions. Also note the slightly raised bumpiness. There are areas of normal skin between. This patient likely complains of intense itching and burning but not necessarily more pain deeper in the skin, fevers or drainage. This is an example of an allergic contact dermatitis and is a reaction to the skin glue or steri strip adhesive coating. The glue dripped on the left side so it looks like a long trail of rash. The first thing you will need to do after talking to me is peel off the skin glue or steri strips, to remove the irritant. Then generally the treatment is supportive, with topical itching cream and or over the counter Benadryl until the itching improves. (Image taken from: https://www.mdedge.com/dermatology/article/87888/wounds/allergic-contact-dermatitis-2-octyl-cyanoacrylate)
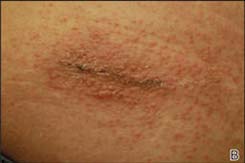
4. Same as above. This is a more close up picture of the skin glue reaction. (Image taken from: https://www.mdedge.com/dermatology/article/87888/wounds/allergic-contact-dermatitis-2-octyl-cyanoacrylate)

5. If you have ever felt a sharp sudden taring sensation or heard a “pop” at your incision and felt a lot of pain, like worse than any pain up to that point, then you may have torn a deep stitch. Subsequently if you notice a soft bulge under the incision but the skin is intact and generally without redness and warmth, then you may have an acute incisional hernia. This could be an emergency. It could also be a deeper infection or an abscess, but you will usually have skin warmth, redness and constant pressure or sharp pain. Lastly it could be a simple seroma, or non-infected natural fluid, built up under the incision. Only a doctor can help determine the difference between these problems and we may need to do a CT scan or ultrasound evaluation to confirm this. (Image taken from: https://www.hernia.ae/incisional-ventral-hernia/)
Infections:
Usually incision infections are not apparent until 5-7 days after surgery. If you have redness that is expanding (growing further away from the incision), warmth, new or worse constant incision pain, swelling and or the skin edges have separated with drainage then this is worrisome for an incisional infection. We will likely call in an antibiotic for you until you can see me in clinic. If it seems mild we may insist on seeing you first before starting antibiotics. I try not to over treat with antibiotics.
Follow up:
Your discharge instructions will say, “Follow up with Dr. Danthuluri about 2 weeks after surgery.”
Most of the time you will have to call yourself and schedule an appointment time that is convenient for you. I typically ask you or family to go ahead and call and schedule while you are waiting to be discharged from the hospital so you do not forget. You can also call once home. If you had an appointment made before surgery I still recommend you call and double check. I may have made decisions in surgery that will alter the follow up time period. For example, If you have staples in your incisions, drains or open wounds which you were not expecting, then most likely I will need to see you sooner than 2 weeks. It is ideal to get staples out in 5-7 days after surgery most of the time. So if you have an appointment that you think is too long after surgery and you are unsure, then please call and ask the schedulers to verify with me when your follow up should be. Basically call our office anytime within 1-3 days after surgery to make or confirm the appointment.
If you happen to have many medical problems and are on multiple medications then I recommend that you call your primary care doctor for a follow up appointment 1-2 weeks after surgery as well. The stress of surgery, change in diet, change in activity levels and the energy demands on the body during recovery may alter your medical conditions. Previously well controlled conditions like diabetes and hypertension may no longer be controlled. A common scenario is loss of diabetes, or blood sugar, control after surgery. Most people have a few days of elevated blood sugars after surgery. Also blood pressures can vary. You may need to hold certain medications or change the doses while you recover. This is especially true after weight loss surgery. So, if you have medical conditions or a special medical need, then plan to visit your primary care doctor as well after surgery.
A good general rule for my diabetic patients is to check the blood glucoses regularly. If you have two checks in a row where the blood glucose is over 200 and not responding to your normal medications, or doses of insulin, then you will need to call your primary care doctor to adjust the medications or add medications. Similarly if you are a long time hypertension patient you can check your blood pressure after surgery. If it is consistently over 160 mmHg or under 90mmHg systolic (the top number) or over 100mmHg or under 60mmHg diastolic (bottom number) then also plan to call and update your primary care doctor and seek advice. If you can not reach them for any reason, please notify our office as well.
Remember this is a general guide. It will serve you well in most cases but every patient and patient need is unique. Do not hesitate to communicate with me if you have any doubts or concerns. My staff and I are here for you no matter what.
Again, thank you or trusting me in your care! I hope you have a smooth and fast recovery.
